Since 1975, Lyme disease has been diagnosed in 49 of the U.S. states, with almost 300,000 cases a year, mostly in the Northeast and Midwest.
Black-legged ticks, the disease’s main vector, are now flourishing in areas previously devoid of the arachnid, including spreading into eastern and central Canada. In 2015, there were more than 700 cases of Lyme disease reported to the Public Health Agency of Canada, up from roughly 130 in 2009.
As a matter of fact, in April 2017, infectious disease expert Tara Moriarty, an associate professor in the faculties of dentistry and medicine at the University of Toronto said that partly thanks to climate change, almost 80 percent of the Canadian population in eastern and central Canada will be living in the habitat of potentially-infected ticks in the near future.
Getting diagnosed and treated is difficult
Tick bites have become so common in Quebec that last month, Quebec’s wildlife protection agents asked the government to officially recognize Lyme disease as a workplace health hazard. It seems that under the current rules, agents who get the disease have to fight with the Workplace Health and Safety Board for access to compensation or care.
“We have to be careful when we go out — wear long clothing and insect repellent,” said Dr. Geneviève Barron, a professor at Université de Sherbrooke, who works with health officials in the Eastern Townships. Barron says the responsibility shouldn’t be on the employee if they get the disease.
But even more worrisome is the number of people in Canada who have been infected with Lyme Disease and are unable to get a doctor to recognize and treat the infection. Undark.org. relates the story of a Manitoba woman who contracted Lyme Disease a couple years ago. She does not remember having the tell-tale bull’s eye rash often seen at the tick-bite site.
Her husband had grown up in New York’s Hudson Valley and recognized the symptoms. Canadian doctors were not convinced. “Even though we had been telling people for months that she had Lyme disease and that all she needed was about four weeks of antibiotics, we were seeing specialist after specialist, and getting the same run-around,” the husband said.
The couple eventually paid “thousands of dollars for testing at a certified lab in the United States, which finally convinced a Canadian doctor to treat her,” he said.
Diagnosis is not straightforward
And even though the tick-borne disease is becoming more prevalent in Canada, it doesn’t mean the medical community has kept pace with the level of risk. “Physicians are confused, still, about how they should be diagnosing it,” Moriarty said.
“If someone has had a tick bite, doctors should administer a protective dose of antibiotics, she said. “That information is not quite getting out there … we need to improve early measures on the part of physicians.”
Earlier in 2017, Dr. Gregory Taylor, the country’s then-chief public health officer, acknowledged that clinicians in Canada are divided on how to interpret the blood test for Lyme disease — and how to treat it. And this is something that needs to be changed now.
“Patients who suspect that they have Lyme disease, and who know that they’ve been bitten by a tick, should be able to go to their doctor and request — within 72 hours of the bite — a dose of antibiotics,” added Moriarty.
Lyme Disease is caused by a bacteria
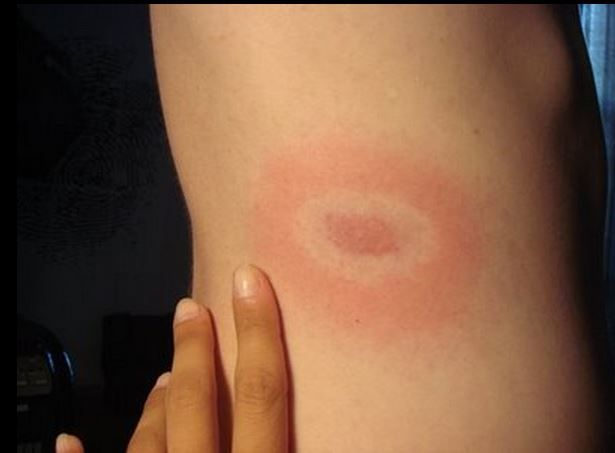
Lyme disease is caused by the bacterium Borrelia burgdorferi and is transmitted to humans through the bite of infected blacklegged ticks. Typical symptoms include fever, headache, fatigue, and a characteristic skin rash called erythema migrans, or what is known as the “bull’s eye rash.”
If left untreated, the infection can spread to joints, the heart, and the nervous system, creating long-term effects on a person’s health. Interestingly, while it is believed that long-term courses of antibiotics are needed to treat the disease, Studies funded by the National Institutes of Health (NIH) have not shown that people who received prolonged courses of antibiotics do better in the long run than people treated with placebo. Actually, this type of treatment can lead to serious side-effects.
Laboratory tests needed for diagnosis
The Centers for Disease Control and Prevention (CDC) recommends a two-step process when testing blood for evidence of antibodies against the Lyme disease bacteria. Both steps can be done using the same blood sample.
In the first step, a testing procedure called “EIA” (enzyme immunoassay) or rarely, an “IFA” (indirect immunofluorescence assay) is done. If this test is negative, no further testing needs to be done. If the first test is positive or indeterminate (sometimes called “equivocal”), then a second test is done.
The second test is more specific and is called an immunoblot test, commonly, a “Western blot” test. Results are considered positive only if the EIA/IFA and the immunoblot are both positive. The tests have been designed to be done together. Skipping the first test and going directly to the Western Blot test could give you false positive results that could lead to misdiagnosis and improper treatment.